IVF: 25 Years On
Twenty five years ago the world’s first in vitro fertilization (IVF) baby was born in England. Since then over a million babies have been born by IVF or other types of Assisted Reproductive Technologies (ART). While it is natural that infertile couples should seek such measures to have a child, there have been many voices raised expressing concern about the procedures. Plenty of social and ethical questions come to mind.
But the medical and physical problems alone should give us pause for concern. A good example was featured on a recent Catalyst program on ABC. Aired on 17 July, the program featured an Australian researcher who has found that IVF kids are twice (and possibly even three times) as likely to have birth defects as normal births.
West Australian epidemiologist, Dr Carol Bower, has found that there are a range of problems associated with IVF, and that it may not be the miracle cure we hoped it would be. Her report indicates that such defects aren’t a one off, but may in fact be a fundamental problem with IVF.
Says Dr Bower, “We’ve seen the whole range of birth defects so far up to one year of age. Heart defects are common… chromosomal abnormalities like Down Syndrome, spina bifida, gastro-intestinal abnormalities, musculo-skeletal, dislocated hips. Club feet, those sorts of thing.”
Other problems also occur: “IVF babies have a lower birth weight, they’re often born pre-term, and we know that cerebral palsy’s more common amongst these children. I mean, it’s not that surprising that they also have a higher rate of birth defects.”
And long term problems also abound: “The sorts of things that are picked up over a year of age are internal abnormalities, renal abnormalities, abnormalities of the bladder, for example. Sometimes some gastro-intestinal abnormalities.” Indeed, many of the abnormalities do not come to light until a later date.
Embryologist Dr. Jeremy Thompson, Head of Reproductive Medicine at the University of Adelaide, says that very little research has gone into this area: “The consumer basis for the industry has been focused on having high pregnancy rates, getting people pregnant as quickly as they possibly can. And quite rightly so from that consumer perspective. But it hasn’t focused necessarily on the long-term outcomes.”
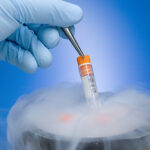
Dr Thompson, whose background is studying IVF in animals, has been aware of problems associated with animals born by IVF. He believes the culture environment may be responsible, at least in part. As the reporter, Jonica Newby explains, “In IVF, for both animals and humans, male sperm is mixed into female’s eggs in a dish. The result, a fertilised embryo is then left to grow in a nutrient culture for 2-5 days, before it’s placed back in the womb. The culture is a liquid mixture of: protein, antioxidants, salts and amino acids.”
She continues, “Disturbingly Jeremy found that even subtle changes in the culture recipe altered the turning on of key genes which could result in abnormal development. And yet, IVF clinics don’t use one standard culture recipe. The culture media is the life support of the IVF embryo in it’s first days of life. It’s amazing it’s never been studied this way till now.”
Dr Thompson admits that things might have been done differently: “I guess in hindsight yes you can say that we should have probably investigated these things before. But it’s only really now that we’ve started to understand what it is about the environment that is having these effects.”
Other medical problems
In addition to the problems highlighted on the Catalyst program, there are many other medical problems associated with IVF and ART. One is the very high failure rate of the technologies involved. Even with some improved success rates over the years, IVF is still only successful in about 10 to 15 per cent of all attempts. And the real issue, not often discussed, is that the original condition remains. Infertile couples remain infertile after the procedure.
Professor Robyn Roland of Deakin University puts it this way: “An enormous problem is that the great majority of women are not going to have babies. When they leave the program, they’re told bye-bye, and there’s no follow-up, no counselling. They’re left with an enormous sense of failure.”
But IVF may have been over-hyped. Many couples who appear to be infertile actually can go on to conceive naturally. Bio-ethicist Nick Tonti-Filippini argues that 50 per cent of couples who believe they are infertile will become pregnant without IVF in five years. If you add IVF to the equation, the figure goes up to 60 per cent, so there is only help of around 10 per cent.
But every publicized success in ART makes many couples with marginal infertility that much more impatient. Such couples should really be considered “sub-fertile” argues science writer Pete Moore: “They are not incapable of having children without assistance, but it might just take a bit longer than for other couples. Rather than waiting two or three years before turning for help, it is now common for couples to approach their doctors after only a few months of unprotected intercourse, anxious that they are infertile. An American survey suggested that concern about fertility problems has risen, despite the fact that the actual age-adjusted incidence of impaired fertility remained stable.”
There are many physical problems associated with IVF. The death rate of newborn IVF babies is around 11 per thousand, which is much higher than the national average.
Moreover, IVF leads to other problems. Around 2 in 5 IVF births are multiple births. Indeed, this problem has become so pronounced that leading Australian obstetricians have called for all IVF patients to be offered single rather than double embryo implantation, and for the monitoring of fertility drugs.
Also, IVF results in a higher rate of premature births, which are often associated with mental and physical retardation, and sometimes death. And while major congenital handicaps are reported in 1.5 per cent of normal conceptions, the figure rises to 2.2 per cent in IVF births.
Other problems can be noted. For example, a Swedish study, reported in the Lancet, found that the high prevalence of twin and triplet pregnancies associated with IVF is linked to developmental problems and neurological complications in the IVF babies. The study found that fertility treatment can triple the chances of a child being born with cerebral palsy. And a recent study by researchers in Perth found that “babies conceived by IVF are more than twice as likely to suffer major birth defects as babies conceived naturally”.
One procedure, in which a single sperm is injected into an egg (ICSI), is said to result in delayed mental development of the children. Research undertaken at a Sydney hospital found that some of children conceived by this type of IVF had a “mild delay in mental development”.
Not only are there risks to the children conceived by IVF, but there are also risks for the mothers. For example, a Stanford University study found that women who had been treated for infertility were three times more likely to develop ovarian cancer than women who were not.
And IVF seems to pass on defects, according to experts. A reproductive biologist at the Royal Women’s Hospital in Melbourne warned that the problem of infertility could be passed on from fathers to sons and bypass an important natural screening process. Professor Roger Short said that we are “bypassing an important safety check of nature’s designing. Evolutionary biologists would have to say that the evidence suggests infertility is not an accident, it’s a protective mechanism and we’re bypassing it at our peril”.
Other problems can be traced to human error, but they are problems nonetheless. There is the somewhat rare, but nonetheless tragic, problem of IVF mix-ups. That is, sperm, eggs, or embryos, are somewhere along the line mixed up, resulting in the wrong children given to the wrong parents. The most recent example took place in Britain when a white couple had black twins following an IVF mix-up.
But such problems are not just due to accidents. Sometimes they are deliberate. Consider the case of an English embryologist who claimed to place embryos in eight women when in fact he had not. He simply performed the operations to help pay off his debts.
Other examples of IVF blunders have taken place over the years. Melbourne’s top IVF experts admitted that the process is not fail-safe, and have revealed that a new genetic test, costing couples $2000, will soon be available to help prevent such mistakes from occurring in the future.
Also, even though it is claimed that the IVF technique is getting better results as time goes on, the prospect is bleak for older women, with women over 40 still having great difficulties conceiving. They experience only a 3 to 5 per cent chance of achieving a live birth through standard IVF procedures. And there is an 80 per cent chance of miscarriage for women who try IVF between the ages of 42 to 45.
And there is a further medical problem. Because so many women think that they can use ART to help them if need be, more and more women are delaying childbearing. But there has been a cost to such waiting. Birth defects are increasing because of these delays. A ten-year study of Victorian births has found that the later age in child birth is correlated with an increase of birth defects.
For these and other reasons, IVF is not a very safe or a very effective medical technology. After 25 years, we may have much less to celebrate than was first imagined.
[1600 words]