
The Vital Necessity of Informed Medical Consent
Numerous human rights declarations speak out against coercive medicine:
Since the horrors of WWII, and the diabolical things done by the Nazis – including the German medical and scientific communities – there have been a slew of various human rights declarations, health acts, and ethics codes written around the world. Many of them seek to counter and offset the sorts of things that were done in Nazi Germany.
A common theme found in almost all of them is that there should be no coercion or compulsion in medical treatment, and full informed consent should be insisted upon. Before any medical treatment or intervention is undertaken, a person must first give consent – without any coercion or manipulation.
This vitally important principle seems to have been thrown out the window by far too many politicians, leaders, governments and businesses during the Covid crisis, especially in regard to mandatory vaccinations. Many states are simply demanding that people get the jab – end of story. And numerous businesses and companies are doing the same.
Not only is this creating a new medical apartheid, a two-tiered society with a health underclass, but it goes against these vital human rights charters and ethics declarations. Places like Australia – where much of this medical coercion and health segregation is taking place – happen to be signatories to many of these covenants and declarations. Indeed, at both federal and state levels Australia also has its own acts and declarations on these things.
Here I offer the relevant portions of ten of these important charters and acts: six international and four Australian:
The Nuremberg Code, 1947
The first of its ten points says this:
The voluntary consent of the human subject is absolutely essential. This means that the person involved should have legal capacity to give consent; should be so situated as to be able to exercise free power of choice, without the intervention of any element of force, fraud, deceit, duress, overreaching, or other ulterior form of constraint or coercion; and should have sufficient knowledge and comprehension of the elements of the subject matter involved as to enable him to make an understanding and enlightened decision. This latter element requires that before the acceptance of an affirmative decision by the experimental subject there should be made known to him the nature, duration, and purpose of the experiment; the method and means by which it is to be conducted; all inconveniences and hazards reasonably to be expected; and the effects upon his health or person which may possibly come from his participation in the experiment. The duty and responsibility for ascertaining the quality of the consent rests upon each individual who initiates, directs, or engages in the experiment. It is a personal duty and responsibility which may not be delegated to another with impunity. media.tghn.org/medialibrary/2011/04/BMJ_No_7070_Volume_313_The_Nuremberg_Code.pdf
The Declaration of Geneva, 1948
This very brief declaration has been updated at various times, and the current 2017 version list 13 points, the first three being:
AS A MEMBER OF THE MEDICAL PROFESSION:
I SOLEMNLY PLEDGE to dedicate my life to the service of humanity;
THE HEALTH AND WELL-BEING OF MY PATIENT will be my first consideration;
I WILL RESPECT the autonomy and dignity of my patient;
https://www.ama.com.au/position-statement/wma-declaration-geneva-2017
The Declaration of Helsinki, 1964
The World Medical Association Declaration of Helsinki – “Ethical Principles for Medical Research Involving Human Subjects” – has also been revised many times since it first appeared. In sections 25-32 it speaks about “informed consent”. Here are the first several of these:
25. Participation by individuals capable of giving informed consent as subjects in medical research must be voluntary. Although it may be appropriate to consult family members or community leaders, no individual capable of giving informed consent may be enrolled in a research study unless he or she freely agrees.
26. In medical research involving human subjects capable of giving informed consent, each potential subject must be adequately informed of the aims, methods, sources of funding, any possible conflicts of interest, institutional affiliations of the researcher, the anticipated benefits and potential risks of the study and the discomfort it may entail, post-study provisions and any other relevant aspects of the study. The potential subject must be informed of the right to refuse to participate in the study or to withdraw consent to participate at any time without reprisal. Special attention should be given to the specific information needs of individual potential subjects as well as to the methods used to deliver the information.
After ensuring that the potential subject has understood the information, the physician or another appropriately qualified individual must then seek the potential subject’s freely-given informed consent, preferably in writing. If the consent cannot be expressed in writing, the non-written consent must be formally documented and witnessed.
All medical research subjects should be given the option of being informed about the general outcome and results of the study.
27. When seeking informed consent for participation in a research study the physician must be particularly cautious if the potential subject is in a dependent relationship with the physician or may consent under duress. In such situations the informed consent must be sought by an appropriately qualified individual who is completely independent of this relationship. https://www.wma.net/what-we-do/medical-ethics/declaration-of-helsinki/
The International Covenant on Civil and Political Rights, 1966, 1976
Here is Article 7 of this covenant:
“No one shall be subjected to torture or to cruel, inhuman or degrading treatment or punishment. In particular, no one shall be subjected without his free consent to medical or scientific experimentation.” https://www.ohchr.org/en/professionalinterest/pages/ccpr.aspx
The Universal Declaration on Bioethics and Human Rights, 2005
Here are parts of this document:
Article 6 Any preventive, diagnostic and therapeutic medical intervention is only to be carried out with the prior, free and informed consent of the person concerned, based on adequate information. The consent should, where appropriate, be express and may be withdrawn by the person concerned at any time and for any reason without disadvantage or prejudice.
Article 9 The privacy of the persons concerned and the confidentiality of their personal information should be respected. To the greatest extent possible, such information should not be used or disclosed for purposes other than those for which it was collected or consented to, consistent with international law, in particular international human rights law.
Article 11 No individual or group should be discriminated against or stigmatized on any grounds, in violation of human dignity, human rights and fundamental freedoms. http://portal.unesco.org/en/ev.php-URL_ID=31058&URL_DO=DO_TOPIC&URL_SECTION=201.html
The U. S. Food and Drug Administration
This is what the FDA has to say about “What is an Emergency Use Authorization (EUA)?”:
An Emergency Use Authorization (EUA) is a mechanism to facilitate the availability and use of medical countermeasures, including vaccines, during public health emergencies, such as the current COVID-19 pandemic. …
How will vaccine recipients be informed about the benefits and risks of any vaccine that receives an EUA?
FDA must ensure that recipients of the vaccine under an EUA are informed, to the extent practicable given the applicable circumstances, that FDA has authorized the emergency use of the vaccine, of the known and potential benefits and risks, the extent to which such benefits and risks are unknown, that they have the option to accept or refuse the vaccine, and of any available alternatives to the product. Typically, this information is communicated in a patient “fact sheet.” The FDA posts these fact sheets on our website. https://www.fda.gov/vaccines-blood-biologics/vaccines/emergency-use-authorization-vaccines-explained
The Victorian Charter of Human Rights and Responsibilities Act 2006
Section 10 of the Act says this:
Protection from torture and cruel, inhuman or degrading treatment
A person must not be—
(a) subjected to torture; or
(b) treated or punished in a cruel, inhuman or degrading way; or
(c) subjected to medical or scientific experimentation or treatment without his or her full, free and informed consent. http://www5.austlii.edu.au/au/legis/vic/consol_act/cohrara2006433/
The NSW Anti Discrimination Act
It says this about “Infectious diseases discrimination”:
What is infectious diseases discrimination?
Infectious diseases discrimination is against the law.
It is when you have been treated unfairly because:
-you have an infectious disease
-people think you have an infectious disease
-you used to have an infectious disease
-you may acquire an infectious disease in the future
-you are the friend, relative or colleague of a person with an infectious disease.
Indirect discrimination is also against the law. This is when there is a rule or requirement that is the same for everyone but unfairly affects people with infectious diseases, and is not reasonable in the circumstances. https://antidiscrimination.nsw.gov.au/anti-discrimination-nsw/discrimination/types-of-discrimination/infectious-diseases-discrimination.html
Australian Regulatory Guidelines for Advertising Therapeutic Goods, 2018
Here is what it says about “Guidance for advertisers”:
This guidance for advertisers applies to the Therapeutic Goods Advertising Code (No.2) 2018. To assist advertisers with implementation, we have also published guidance material: Complying with the Therapeutic Goods Advertising Code (No. 2) 2018. Version 2.8, October 2020
Advertising vaccination services
We do not regulate the advertising of health services but if your advertisement for a vaccination
service also promotes the use of a therapeutic good it is considered an advertisement for a
therapeutic good which, outside of the context described above, would be likely to contravene
the Act.
What to avoid when advertising vaccination services
When advertising vaccination services, avoid using:
– information that might enable consumers to identify the particular vaccine or the manufacturer of the vaccine provided with the service
– statements or representations that harmful effects will occur from not receiving the vaccine
– references to any misleading therapeutic benefit of a vaccine (for example, a use that is not a TGA-approved indication for the vaccine)
– an indication that the vaccine administered as part of the service is superior to other vaccines
-portrayals of the vaccine or service in a way that trivialises or conflicts with public health policies, or misleads consumers in any other way
-price comparisons
– incentives to encourage the consumer to obtain the service or vaccine, or
– any other claim that promotes the use or supply of the vaccine Use of any of the above makes advertising of your service to be more likely considered advertising of the vaccine itself and subject to therapeutic goods legislation. https://www.tga.gov.au/sites/default/files/australian-regulatory-guidelines-advertising-therapeutic-goods-argatg.pdf
The Australian Immunisation Handbook (from the Australian Government Department of Health)
Relevant portions of the Handbook are these:
Valid consent is the voluntary agreement by an individual to a proposed procedure, which is given after sufficient, appropriate and reliable information about the procedure, including the potential risks and benefits, has been conveyed to that individual.
As part of the consent procedure, people receiving vaccines and/or their parents or carers should be given sufficient information (preferably written) about the risks and benefits of each vaccine. This includes:
-what adverse events are possible
-how common they are
-what they should do about them
Criteria for valid consent
For consent to be legally valid, the following elements must be present:
-It must be given by a person with legal capacity, and of sufficient intellectual capacity to understand the implications of receiving a vaccine.
-It must be given voluntarily in the absence of undue pressure, coercion or manipulation.
-It must cover the specific procedure that is to be performed.
-It can only be given after the potential risks and benefits of the relevant vaccine, the risks of not having it, and any alternative options have been explained to the person.
-The person must have the opportunity to seek more details or explanations about the vaccine or its administration.
-The information must be provided in a language or by other means that the person can understand. Where appropriate, involve an interpreter or cultural support person.
-Obtain consent before each vaccination, after establishing that there are no medical condition(s) that contraindicate vaccination. Consent can be verbal or written. immunisationhandbook.health.gov.au/vaccination-procedures/preparing-for-vaccination
As these and other documents make clear, the sorts of things we are seeing in Australia and the West concerning mandatory medicine, coercive health care, forced injections, vaccine passports and the like are for the most part condemned as unethical and gross infringements on our basic human rights and fundamental civil liberties.
[1986 words]



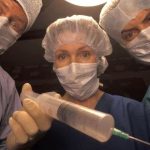







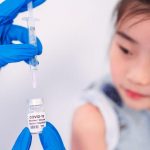






The no jab no job mandates are nearly upon us. My profession requires jabs to attend building sites in Victoria and it appears NSW new “open up” proposal applies only to those jabbed.
In Qld it’ll only be a matter time before similar “no jab, no site entry” rules will apply. I will accept a genuine COVID vaccination in the legal definition, not the experimental gene therapy mRNA injection being passed off as. sars-2 COVID “vaccine”
If I lose my job, so be it which will be a disappointment since as a 66 yo, took me 12 months to find.
I will not have chimeric sars-2 DNA incorporated into my DNA and if that makes me a second class citizen, so be it. Better to die free than live un bondage to medical racism,,
Thanks Philip. Millions of people in the once free West face the very same predicament. Yet the covid alarmists and zombies are still quite happy to lie to us, claiming there is nothing mandatory here – it is all free choice! Yeah right. When those who have valid reasons to be hesitant about it are kicked out of their jobs, denied the ability to feed their own families and earn a living, are prevented from getting the most basic of goods and services, they are NOT at all free to chose. “Get the jab or starve to death” is basically the demand being made by so many in both business and government. Um, what part of this do these fools going on about choice not understand?: “It must be given voluntarily in the absence of undue pressure, coercion or manipulation?”
Unfortunately, all those documents are not worth the paper they are written on. As I have mentioned here, QPS and Qld Health do not even give their staff the opportunity to express their consent or otherwise. I’m sure it is or will be the same for every other department or employer. There are no government bodies challenging them on behalf of the people they represent. If we have a ‘Christian’ Prime Minister supporting all of this and not speaking up
Unless you have unlimited funds to take it to court (or a generous lawyer) and you happen to get a judge that rules on the law and not activist and pro-government principles, there is not likely to be any success in challenging the actions of governments and employers.
We can only pray for a miracle that circumstances show up these tyrants for what they are and that the narrative unravels.
The only comfort we can take is that God is a fair judge and His judgement on those who willingly subject people to these experimental treatments will be fitting and eternal.
Yes Troy, many of these documents seem to mean very little to our leaders.
Please note that “chimeric sars-2 DNA” is not “incorporated into my DNA” by current inoculations. The genome is not altered. If one is basing acceptance or refusal of the inoculations on the question how they work it would be best to be clear how they work.
Dear Bill,
World so called ‘leaders’! Wimps would be a better word for them are obviously taking no notice of these declarations but thank you Bill for informing us about them anyway.
Let’s hope that making vaccinations mandatory for Australian employees will eventually backfire on those firms who insist on it. This is because there is already a shortage of labour because of border closures and travel bans on students, backpackers and tourists. Students and backpackers in particular made up a big part of the casual labour force.
A few weeks ago I had my hair cut at a walk in hairdressers whose manager apologised for keeping me waiting as he only had one young lad as hairdresser who was going like the bees wings. He said he had been unable to hire any more staff even though he had a notice in the window. The baker opposite was in the same position.She said she had been working a fourteen hour day because of staff shortages.
This might have had something to do with the job seeker payment as well. However, firms might be too confident that they can get enough workers because people might become fed up and distrustful of the vaccinations especially as the so called health experts are claiming that the vaccinated will require regular booster shots.
Troy Hartley is right. All these fine sounding statements are not worth a prince of salt. And Morrison? What can you say. He is as weak as water. I used to pray for him. Now I pray he will just move aside. His latest cave in on Climate change is a disgrace. Its all so depressing.
This is the way out for those who have been affected (and who hasn’t) by the angst we see on a daily basis due to this tyrannical over-reach of government…
Trust this will help someone in your circle.
Stand Firm, Hold the Line and Focus on Jesus – ONLY those who are fixated on & living in Him will stay strong….Look Up and Live…
https://www.reignitedemocracyaustralia.com.au/vaccine-exemption/
Thanks Melinda.
I am proud of our two sons who are 19 & 21, standing up for the truth even it means they lose their jobs. They are hard working healthy young men like many others who stand firm believing that something good will come out of this. It is hard. God willing, we will soldier on.
Keep standing strong Yuzuri.
Thanks again Bill for the info & for staying strong…..what times we are in ?! And not by the hand of some far off despotic regime but by our own elected so called “ leaders “. Woe to them who call evil, good etc
Thanks Richard.
My first comment in a while.
It’s interesting that you cited the AMA regarding the Geneva Declaration.
I clicked on the link, their latest article is on “Anti-vaccine misinformation”.
They have become strongly pro-vax, in line with government agencies.
I resigned from them in late 2017, after being a member for over 30 years, on principle, as they supported SSM, & I could no longer be a member on principle.
Links to their website show their latest policy on LGBTIA+ (whatever)